Nephrin研究的机遇和挑战(上)
——
未明原因的pFSGS
近来研究显示,抗-Nephrin自身抗体(Anti-nephrin Ab)在微小病变(MCD)和局灶性节段性肾小球硬化(FSGS)的发生中扮演重要的作用,本文概述了抗-Nephrin抗体作为MCD和原发性FSGS(pFSGS)的血液循环渗透因子的研究进展,并对将来的研究方向提出了展望。
循环因子理论与FSGS
当1972年Hoyer等[6]第一次报道了肾移植术后复发FSGS的患者开始,研究人员就推测血液中某种循环渗透因子可能引起了FSGS的产生。随之流行病学研究显示,移植后FSGS具有较高的复发率,有时在移植后几小时内就会发生,这结果进一步促使研究人员相信,致病因子可能不是“肾脏内的局部现象”,而是一种血液循环渗透因子,它通过改变肾小球屏障来损伤足细胞[7-8]。直到2012年Gallon等[9]在一个FSGS复发的患者案例研究中发现,当移植肾被切除并再次移植给另一个没有FSGS病史的受者时,肾脏的功能得到了恢复,且FSGS特有的组织病理学损害也发生了逆转,这基本确定了是血液中存在的某些循环渗透因子导致了FSGS的发生。
随后几年,大量的研究资源投入到寻找在MCD和pFSGS蛋白尿形成中起关键作用的循环渗透因子[10-11]。尽管投入了非常大的资源和研究努力,这些未知的循环通透性因子的鉴定一直是艰苦漫长的,研究者并没有找到可靠一致的生物标志物。
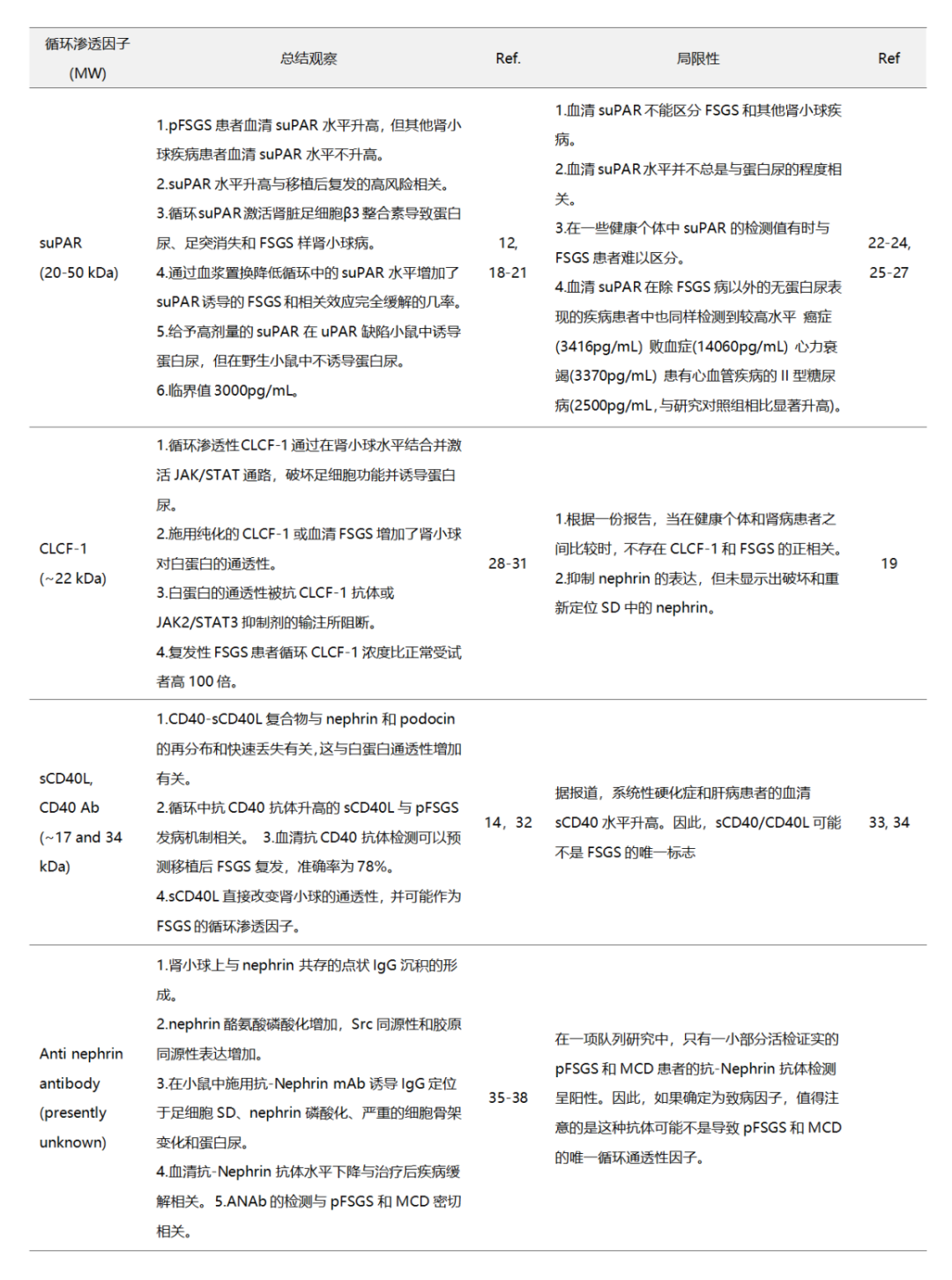
一些被认为增加血清蛋白血管透过性的候选生物标志物分子(表1),包括可溶性尿激酶型纤溶酶原激活物受体(suPAR)[12]、心肌营养素样细胞因子-1 (CLCF-1)[13]、可溶性CD40配体[14]等等,已经发现与MCD和pFSGS的进展和复发相关,但是验证其临床效用的研究表明,这些标记物并不在MCD和FSGS的发展中起到决定性作用,它们也可以在健康人和非肾病综合征患者血清中检测到[15-17]。
表1. FSGS和MCD相关循环渗透因子及其局限性
Nephrin蛋白介绍
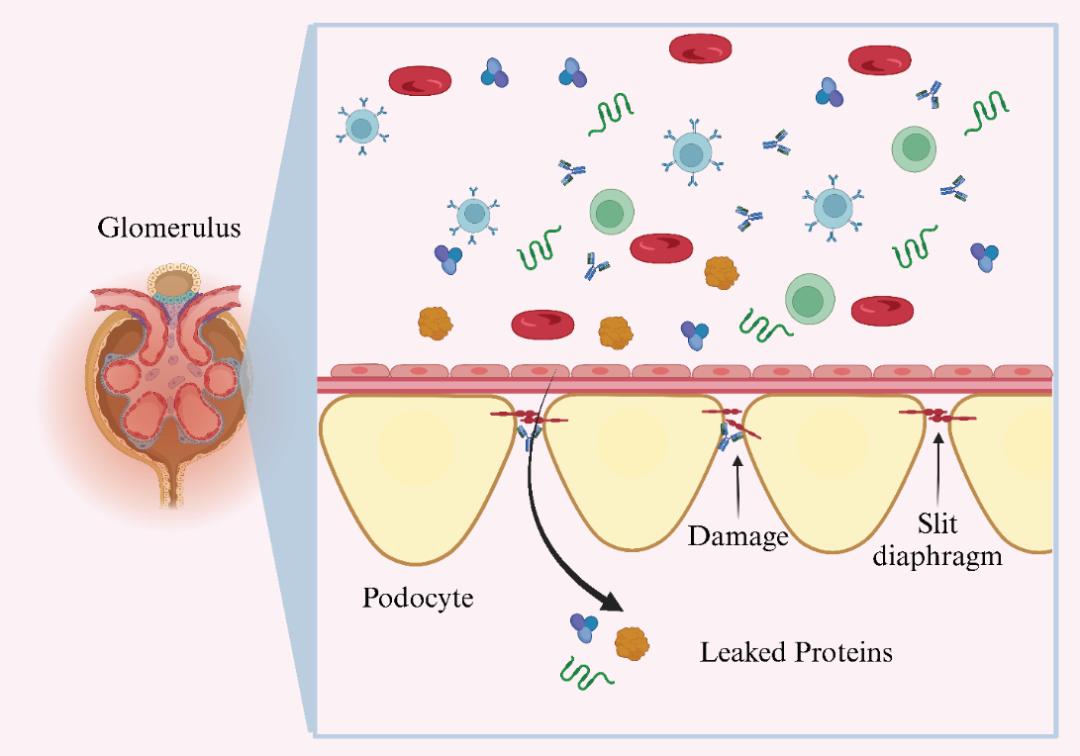
1966年,在一组患有先天性肾病综合征(NPHS1)[39]的芬兰家系中,研究发现这是一种罕见的遗传基因突变造成的肾脏疾病,但导致这种疾病的具体基因未知。直到1998年NPHS1基因所在的关键染色体区域被鉴定和测序, NPHS1基因的表达产物被命名为Nephrin,其基因座定位于染色体19q12-q13.1[40-41]。虽然Nephrin蛋白的精确结构和功能在此时仍然未知,但据推测,其结构域结构类似于属于免疫球蛋白家族的一大类细胞粘附受体,它可以作为粘附受体和信号蛋白[40]发挥作用。在后续研究中[42-43],证实Nephrin是形成足细胞裂孔隔膜相关复合物(slit diaphragm, SD)的组成部分,其与肾小球内皮细胞和基底膜(GBM)一起形成肾小球滤过屏障。(图1)
图1. Nephrin抗体诱导纵膈改变、足细胞损伤和蛋白质渗漏入尿液中
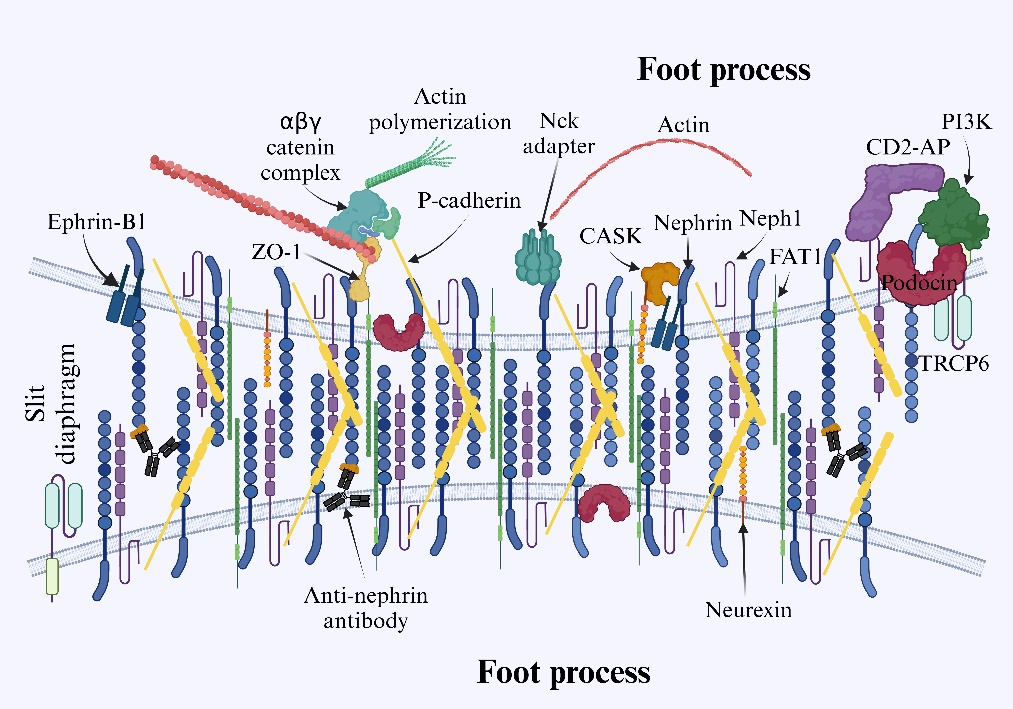
Nephrin是一种跨膜蛋白,其N-末端为胞外片段,C-末端为胞内结构域,使用对人Nephrin的N-末端特异的抗体检测证实了其位于肾的纵膈[44]。整个蛋白由八个免疫球蛋白样胞外结构域、一个纤连蛋白III型样结构域、一个跨膜结构域和一个短的胞内结构域组成,它通过与肌动蛋白细胞骨架[40,45]的相互作用而维持足细胞的组织形态结构和功能。作为免疫球蛋白超家族的细胞表面受体蛋白,Nephrin还参与细胞间粘附和信号传导功能。当Src激酶家族的Fyn磷酸化Nephrin的胞内结构域的六个酪氨酸残基(Tyr1114、Tyr1136、Tyr1176、Tyr1183、Tyr1193、Tyr1217)中的一个或多个时,由Nephrin的胞内尾部介导的下游信号传导被激活[46]。具体表现为磷酸化的胞内结构域会与几种足细胞胞质蛋白相互作用,包括podocin、CD2AP、NEPH1和磷脂酰肌醇3-激酶(PI3K),以将下游信号传递到肌动蛋白细胞骨架,从而调节足细胞的结构完整性和肾小球滤过狭缝的功能[47-48]。磷酸化Nephrin促进Nck衔接蛋白、ZO-1、连环蛋白、桶蛋白、足细胞素、CD2-AP和PI3K等的募集并与之相互作用,Nck衔接蛋白发出肌动蛋白重塑的信号,并参与多种细胞内信号通路的调节,从而影响对足细胞稳定至关重要的肌动蛋白的聚合动力学[48-49](图2)。
图2. 相邻足突之间的缝隙层示意图。胞内结构域在磷酸化时通过级联反应与胞质蛋白相互作用,诱导信号传递,调节肌动蛋白聚合动力学并调整足细胞结构。抗-Nephrin抗体和Nephrin之间的相互作用通过导致Nephrin远离狭缝层,重新定位而失去狭缝屏障功能。
参考文献

[1]Büscher AK, Konrad M, Nagel M, et al. Mutations in podocyte genes are a rare cause of primary FSGS associated with ESRD in adult patients. Clin Nephrol. 2012;78(1):47-53. doi:10.5414/cn107320
[2]Isaranuwatchai S, Chanakul A, Ittiwut C, Ittiwut R, Srichomthong C, Shotelersuk V, Suphapeetiporn K, Praditpornsilpa K. Pathogenic variant detection rate by whole exome sequencing in Thai patients with biopsy-proven focal segmental glomerulosclerosis. Sci Rep. 2023 Jan 16;13(1):805. doi: 10.1038/s41598-022-26291-y. PMID: 36646731; PMCID: PMC9842604.
[3]Santín S, Bullich G, Tazón-Vega B, et al. Clinical utility of genetic testing in children and adults with steroid-resistant nephrotic syndrome.Clin J Am Soc Nephrol. 2011;6(5):1139-1148. doi:10.2215/CJN.05260610
[4]Gandzali Ngabe, P.E., Bonkano Baoua, D., Lengani, A.H.Y., Yattara, H., Kama Yatte, A., Loumingou, R., Tall, L., Ka, E.F., Niang, A. and Diouf, B. (2023) Focal Segmantal Glomerulosclerosis: Epidemiological, Clinico-Biological, Pathological, Etiological, Therapeutic and Evolutionary Profiles in Dakar. Open Journal of Nephrology, 13, 174-194. doi: 10.4236/ojneph.2023.132017.
[5]Rery TF Yuniarti, Ian Effendi, Zulkhair Ali, Novadian, Suprapti, Elfiani, Novandra AP, Dila Siti Hamidah, Fadil Pramudhya Husein, & Ika Kartika Edi P. (2024). Is It a Tumor or Not? A Case of Focal Segmental Glomerulosclerosis Secondary to Type 2 Diabetes with a Concomitant Renal Pseudotumor.Bioscientia Medicina : Journal of Biomedicine and Translational Research, 8(12), 5801-5813.
[6]Hoyer, J. R., Vernier, R. L., Najarian, J. S., Raij, L., Simmons, R. L., and Michael, A. F., Recurrence of idiopathic nephrotic syndrome after renal transplantation, Lancet, 1972, Vol 2(7773) p. 343-8.
[7]Dantal, J., Baatard, R., Hourmant, M., Cantarovich, D., Buzelin, F., and Soulillou, J. P., Recurrent nephrotic syndrome following renal transplantation in patients with focal glomerulosclerosis: a one-center study of plasma exchange effects, Transplantation, 1991, Vol 52(5) p.
[8]Savin Virginia, J., Sharma, R., Sharma, M., McCarthy Ellen, T., Swan Suzanne, K., Ellis, E., Lovell, H., Warady, B., Gunwar, S., Chonko Arnold, M., Artero, M., and Vincenti, F., Circulating Factor Associated with Increased Glomerular Permeability to Albumin in Recurrent Focal Segmental Glomerulosclerosis, New England Journal of Medicine, 1991, Vol 334(14) p. 878-883.
[9] Gallon, L., Leventhal, J., Skaro, A., Kanwar, Y., and Alvarado, A., Resolution of recurrent focal segmental glomerulosclerosis after retransplantation, N Engl J Med, 2012, Vol 366(17) p. 1648-9.
[10] den Braanker, D. J. W., Maas, R. J., Deegens, J. K., Yanginlar, C., Wetzels, J. F. M., van der Vlag, J., and Nijenhuis, T., Novel in vitro assays to detect circulating permeability factor(s) in idiopathic focal segmental glomerulosclerosis, Nephrology Dialysis Transplantation, 2021, Vol 36(2) p. 247-256.
[11] Gauckler, P., Shin, J. I., Alberici, F., Audard, V., Bruchfeld, A., Busch, M., Cheung, C. K., Crnogorac, M., Delbarba, E., Eller, K., Faguer, S., Galesic, K., Griffin, S., Hrušková, Z., Jeyabalan, A., Karras, A., King, C., Kohli, H. S., Maas, R., Mayer, G., Moiseev, S., Muto, M., Odler, B., Pepper, R. J., Quintana, L. F., Radhakrishnan, J., Ramachandran, R., Salama, A. D., Segelmark, M., Tesař, V., Wetzels, J., Willcocks, L., Windpessl, M., Zand, L., Zonozi, R., and Kronbichler, A., Rituximab in adult minimal change disease and focal segmental glomerulosclerosis - What is known and what is still unknown?, Autoimmunity Reviews, 2020, Vol 19(11) p. 102671.
[12] Wei, C., Trachtman, H., Li, J., Dong, C., Friedman, A. L., Gassman, J. J., McMahan, J. L., Radeva, M., Heil, K. M., Trautmann, A., Anarat, A., Emre, S., Ghiggeri, G. M., Ozaltin, F., Haffner, D., Gipson, D. S., Kaskel, F., Fischer, D. C., Schaefer, F., and Reiser, J., Circulating suPAR in two cohorts of primary FSGS, J Am Soc Nephrol, 2012, Vol 23(12) p. 2051-9.
[13] Sharma, M., Zhou, J., Gauchat, J. F., Sharma, R., McCarthy, E. T., Srivastava, T., and Savin, V. J., Janus kinase 2/signal transducer and activator of transcription 3 inhibitors attenuate the effect of cardiotrophin-like cytokine factor 1 and human focal segmental glomerulosclerosis serum on glomerular filtration barrier, Transl Res, 2015, Vol 166(4) p. 384-98.
[14] Doublier, S., Zennaro, C., Musante, L., Spatola, T., Candiano, G., Bruschi, M., Besso, L., Cedrino, M., Carraro, M., Ghiggeri, G. M., Camussi, G., and Lupia, E., Soluble CD40 ligand directly alters glomerular permeability and may act as a circulating permeability factor in FSGS, PLOS ONE, 2017, Vol 12(11) p. e0188045.
[15] Meijers, B., Maas, R. J. H., Sprangers, B., Claes, K., Poesen, R., Bammens, B., Naesens, M., Deegens, J. K. J., Dietrich, R., Storr, M., Wetzels, J. F. M., Evenepoel, P., and Kuypers, D., The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis, Kidney International, 2014, Vol 85(3) p. 636-640.
[16] Müller-Deile, J., Sarau, G., Kotb, A. M., Jaremenko, C., Rolle-Kampczyk, U. E., Daniel, C., Kalkhof, S., Christiansen, S. H., and Schiffer, M., Novel diagnostic and therapeutic techniques reveal changed metabolic profiles in recurrent focal segmental glomerulosclerosis, Scientific Reports, 2021, Vol 11(1) p. 4577.
[17] Hou, S., Yang, B., Chen, Q., Xu, Y., and Li, H., Potential biomarkers of recurrent FSGS: a review, BMC Nephrology, 2024, Vol 25(1) p. 258.
[18]Wei, C., El Hindi, S., Li, J., Fornoni, A., Goes, N., Sageshima, J., Maiguel, D., Karumanchi, S. A., Yap, H. K., Saleem, M., Zhang, Q., Nikolic, B., Chaudhuri, A., Daftarian, P., Salido, E., Torres, A., Salifu, M., Sarwal, M. M., Schaefer, F., Morath, C., Schwenger, V., Zeier, M., Gupta, V., Roth, D., Rastaldi, M. P., Burke, G., Ruiz, P., and Reiser, J., Circulating urokinase receptor as a cause of focal segmental glomerulosclerosis, Nat Med, 2011, Vol 17(8) p. 952-60.
[19] Chebotareva, N., Vinogradov, A., Cao, V., Gindis, A., Berns, A., Alentov, I., and Sergeeva, N., Serum levels of plasminogen activator urokinase receptor and cardiotrophin-like cytokine factor 1 in patients with nephrotic syndrome, Clin Nephrol, 2022, Vol 97(2) p. 103-110.
[20] da Silva, C. A., Araújo, L. S., Dos Reis Monteiro, M. L. G., de Morais Pereira, L. H., da Silva, M. V., Castellano, L. R. C., Corrêa, R. R. M., Dos Reis, M. A., and Machado, J. R., Evaluation of the Diagnostic Potential of uPAR as a Biomarker in Renal Biopsies of Patients with FSGS, Dis Markers, 2019, Vol 2019 p. 1070495.
[21] Wei, C., Möller, C. C., Altintas, M. M., Li, J., Schwarz, K., Zacchigna, S., Xie, L., Henger, A., Schmid, H., Rastaldi, M. P., Cowan, P., Kretzler, M., Parrilla, R., Bendayan, M., Gupta, V., Nikolic, B., Kalluri, R., Carmeliet, P., Mundel, P., and Reiser, J., Modification of kidney barrier function by the urokinase receptor, Nat Med, 2008, Vol 14(1) p. 55-63. 10.1038/nm1696.
[22] Meijers, B., Maas, R. J. H., Sprangers, B., Claes, K., Poesen, R., Bammens, B., Naesens, M., Deegens, J. K. J., Dietrich, R., Storr, M., Wetzels, J. F. M., Evenepoel, P., and Kuypers, D., The soluble urokinase receptor is not a clinical marker for focal segmental glomerulosclerosis, Kidney International, 2014, Vol 85(3) p. 636-640.
[23] Maas, R. J. H., Wetzels, J. F. M., and Deegens, J. K. J., Serum-soluble urokinase receptor concentration in primary FSGS, Kidney International, 2012, Vol 81(10) p. 1043-1044.
[24] Maas, R. J. H., Wetzels, J. F. M., and Deegens, J. K. J., Serum suPAR concentrations in patients with focal segmental glomerulosclerosis with end-stage renal disease, Kidney International, 2014, Vol 85(3) p. 711.
[25] Maas, R. J. H., Deegens, J. K. J., and Wetzels, J. F. M., Serum suPAR in patients with FSGS: trash or treasure?, Pediatric Nephrology, 2013, Vol 28(7) p. 1041-1048. 10.1007/s00467-013-2452-5.
[26] Hayek, S. S., Tahhan, A. S., Ko, Y.-A., Alkhoder, A., Zheng, S., Bhimani, R., Hartsfield, J., Kim, J., Wilson, P., Shaw, L., Wei, C., Reiser, J., and Quyyumi, A. A., Soluble Urokinase Plasminogen Activator Receptor Levels and Outcomes in Patients with Heart Failure, Journal of Cardiac Failure, 2023, Vol 29(2) p. 158-167.
[27] Mohammed, M. S. and Ahmed, H. S., Plasminogen activator urokinase receptor as a diagnostic and prognostic biomarker in type 2 diabetic patients with cardiovascular disease, J Cardiovasc Thorac Res, 2023, Vol 15(3) p. 154-160. 10.34172/jcvtr.2023.32895.
[28] Sharma, M., Zhou, J., Gauchat, J. F., Sharma, R., McCarthy, E. T., Srivastava, T., and Savin, V. J., Janus kinase 2/signal transducer and activator of transcription 3 inhibitors attenuate the effect of cardiotrophin-like cytokine factor 1 and human focal segmental glomerulosclerosis serum on glomerular filtration barrier, Transl Res, 2015, Vol 166(4) p. 384-98.
[29] Savin, V. J., Sharma, M., Zhou, J., Gennochi, D., Fields, T., Sharma, R., McCarthy, E. T., Srivastava, T., Domen, J., Tormo, A., and Gauchat, J. F., Renal and Hematological Effects of CLCF-1, a B-Cell-Stimulating Cytokine of the IL-6 Family, J Immunol Res, 2015, Vol 2015 p. 714964.
[30] Savin, V. J., McCarthy, E. T., and Sharma, M., Permeability factors in nephrotic syndrome and focal segmental glomerulosclerosis, Kidney Res Clin Pract, 2012, Vol 31(4) p. 205-13.
[31] McCarthy, E. T., Sharma, M., and Savin, V. J., Circulating permeability factors in idiopathic nephrotic syndrome and focal segmental glomerulosclerosis, Clin J Am Soc Nephrol, 2010, Vol 5(11) p. 2115-21.
[32] Delville, M., Sigdel, T. K., Wei, C., Li, J., Hsieh, S. C., Fornoni, A., Burke, G. W., Bruneval, P., Naesens, M., Jackson, A., Alachkar, N., Canaud, G., Legendre, C., Anglicheau, D., Reiser, J., and Sarwal, M. M., A circulating antibody panel for pretransplant prediction of FSGS recurrence after kidney transplantation, Sci Transl Med, 2014, Vol 6(256) p. 256ra136.
[33] Komura, K., Fujimoto, M., Matsushita, T., Yanaba, K., Kodera, M., Kawasuji, A., Hasegawa, M., Takehara, K., and Sato, S., Increased serum soluble CD40 levels in patients with systemic sclerosis, J Rheumatol, 2007, Vol 34(2) p. 353-8.
[34] Liu, H., Qi, C. J., Zhuang, Y. M., Gan, J. H., Li, H. L., Yin, C. S., and Zhang, X. G., [Serum levels and clinical significance of soluble CD40 in liver disease], Xi Bao Yu Fen Zi Mian Yi Xue Za Zhi, 2006, Vol 22(6) p. 738-41.
[35] Chebotareva, N., Vinogradov, A., Birukova, Y., Alentov, I., Sergeeva, N., Chemodanova, D., Kononikhin, A. S., and Moiseev, S. V., A pilot study of anti-nephrin antibodies in podocytopaties among adults, Nephrology (Carlton), 2024, Vol 29(2) p. 86-92.
[36] Hengel Felicitas, E., Dehde, S., Lassé, M., Zahner, G., Seifert, L., Schnarre, A., Kretz, O., Demir, F., Pinnschmidt Hans, O., Grahammer, F., Lucas, R., Mehner Lea, M., Zimmermann, T., Billing Anja, M., Oh, J., Mitrotti, A., Pontrelli, P., Debiec, H., Dossier, C., Colucci, M., Emma, F., Smoyer William, E., Weins, A., Schaefer, F., Alachkar, N., Diemert, A., Hogan, J., Hoxha, E., Wiech, T., Rinschen Markus, M., Ronco, P., Vivarelli, M., Gesualdo, L., Tomas Nicola, M., and Huber Tobias, B., Autoantibodies Targeting Nephrin in Podocytopathies, New England Journal of Medicine, 2024, Vol 391(5) p. 422-433.
[37] Watts, A. J. B., Keller, K. H., Lerner, G., Rosales, I., Collins, A. B., Sekulic, M., Waikar, S. S., Chandraker, A., Riella, L. V., Alexander, M. P., Troost, J. P., Chen, J., Fermin, D., Yee, J. L., Sampson, M. G., Beck, L. H., Jr., Henderson, J. M., Greka, A., Rennke, H. G., and Weins, A., Discovery of Autoantibodies Targeting Nephrin in Minimal Change Disease Supports a Novel Autoimmune Etiology, J Am Soc Nephrol, 2022, Vol 33(1) p. 238-252.
[38] Shirai, Y., Miura, K., Ishizuka, K., Ando, T., Kanda, S., Hashimoto, J., Hamasaki, Y., Hotta, K., Ito, N., Honda, K., Tanabe, K., Takano, T., and Hattori, M., A multi-institutional study found a possible role of anti-nephrin antibodies in post-transplant focal segmental glomerulosclerosis recurrence, Kidney Int, 2024, Vol 105(3) p. 608-617.
[39] Norio, R., Heredity in the congenital nephrotic syndrome. A genetic study of 57 finnish FAMILIES WITH A REVIEW OF REPORTED CASES, Ann Paediatr Fenn, 1966, Vol 12 p. Suppl 27:1-94.
[40] Kestilä, M., Lenkkeri, U., Männikkö, M., Lamerdin, J., McCready, P., Putaala, H., Ruotsalainen, V., Morita, T., Nissinen, M., Herva, R., Kashtan, C. E., Peltonen, L., Holmberg, C., Olsen, A., and Tryggvason, K., Positionally Cloned Gene for a Novel Glomerular Protein—Nephrin—Is Mutated in Congenital Nephrotic Syndrome, Molecular Cell, 1998, Vol 1(4) p. 575-582.
[41] Kestilä, M., Männikkö, M., Holmberg, C., Gyapay, G., Weissenbach, J., Savolainen, E. R., Peltonen, L., and Tryggvason, K., Congenital nephrotic syndrome of the Finnish type maps to the long arm of chromosome 19, Am J Hum Genet, 1994, Vol 54(5) p. 757-64.
[42] Ruotsalainen, V., Ljungberg, P., Wartiovaara, J., Lenkkeri, U., Kestilä, M., Jalanko, H., Holmberg, C., and Tryggvason, K., Nephrin is specifically located at the slit diaphragm of glomerular podocytes, Proc Natl Acad Sci U S A, 1999, Vol 96(14) p. 7962-7.
[43]Topham, P. S., Kawachi, H., Haydar, S. A., Chugh, S., Addona, T. A., Charron, K. B., Holzman, L. B., Shia, M., Shimizu, F., and Salant, D. J., Nephritogenic mAb 5-1-6 is directed at the extracellular domain of rat nephrin, J Clin Invest, 1999, Vol 104(11) p. 1559-66.
[44Holzman, L. B., St John, P. L., Kovari, I. A., Verma, R., Holthofer, H., and Abrahamson, D. R., Nephrin localizes to the slit pore of the glomerular epithelial cell, Kidney Int, 1999, Vol 56(4) p. 1481-91.
[45] Schoeb, D. S., Chernin, G., Heeringa, S. F., Matejas, V., Held, S., Vega-Warner, V., Bockenhauer, D., Vlangos, C. N., Moorani, K. N., Neuhaus, T. J., Kari, J. A., MacDonald, J., Saisawat, P., Ashraf, S., Ovunc, B., Zenker, M., and Hildebrandt, F., Nineteen novel NPHS1 mutations in a worldwide cohort of patients with congenital nephrotic syndrome (CNS), Nephrol Dial Transplant, 2010, Vol 25(9) p. 2970-6.
[46] Denhez, B. and Geraldes, P., "Regulation of Nephrin Phosphorylation in Diabetes and Chronic Kidney Injury", in Protein Reviews: Volume 18, M.Z. Atassi, Editor, Springer Singapore: Singapore. 2017. p. 149-161.
[47] Tian, Y., Chen, X.-m., Liang, X.-m., Wu, X.-b., and Yao, C.-m., SGLT2 inhibitors attenuate nephrin loss and enhance TGF-β1 secretion in type 2 diabetes patients with albuminuria: a randomized clinical trial, Scientific Reports, 2022, Vol 12(1) p. 15695.
[48] Verma, R., Kovari, I., Soofi, A., Nihalani, D., Patrie, K., and Holzman, L. B., Nephrin ectodomain engagement results in Src kinase activation, nephrin phosphorylation, Nck recruitment, and actin polymerization, J Clin Invest, 2006, Vol 116(5) p. 1346-59.
[49] Jones, N., Blasutig, I. M., Eremina, V., Ruston, J. M., Bladt, F., Li, H., Huang, H., Larose, L., Li, S. S. C., Takano, T., Quaggin, S. E., and Pawson, T., Nck adaptor proteins link nephrin to the actin cytoskeleton of kidney podocytes, Nature, 2006, Vol 440(7085) p. 818-823.


